Causes of facial pain. Numerous conditions, including as sinus infections and dental issues, can cause the pain. face injuries, trigeminal neuralgia, and TMJ issues. Finding the root cause of facial discomfort is crucial to putting the right management and treatment plans in place. if you have severe or ongoing facial pain. For an accurate assessment and individualized treatment, it’s critical to speak with a healthcare provider. People can find relief from facial pain and enhance their general quality of life with prompt intervention and thorough management.
CAUSES OF FACIAL PAIN
A distressing condition, facial pain can interfere with eating, speaking, sleeping, and socializing, among other elements of daily living. Although there are many different reasons of facial pain, managing and relieving it effectively requires a grasp of the prevalent causes. The various causes of facial pain will be covered in this article, along with methods for relieving the discomfort.
1. Dental Problems:

Dental issues are a leading cause of pain on the face, with conditions such as tooth decay, gum disease, and dental abscesses contributing to discomfort in the jaw, cheeks, and surrounding areas. Toothaches, jaw stiffness, and pain while chewing or biting are common symptoms of dental-related pain. Regular dental check-ups, proper oral hygiene, and prompt treatment of dental problems are essential for preventing and managing facial pain of dental origin.
2. Sinus Infections:
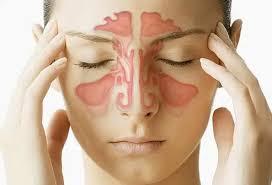
Sinus infections, also known as sinusitis, occur when the sinuses become inflamed and swollen due to infection or inflammation of the sinus tissues. Facial pain associated with sinusitis typically manifests as pressure or tenderness in the cheeks, forehead, and around the eyes. Other symptoms may include nasal congestion, headache, fatigue, and thick nasal discharge. Treatment for sinusitis may include antibiotics, nasal decongestants, saline nasal irrigation, and pain relief medication to alleviate symptoms and clear the infection.
3. Temporomandibular Joint Disorders:
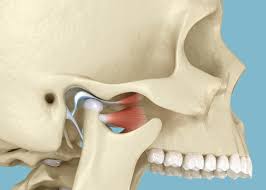
Causes of facial pain
Temporomandibular joint disorders (TMJ disorders) affect the joints that connect the jawbone to the skull, leading to facial pain, jaw stiffness, and difficulty chewing or speaking. TMJ disorders can be caused by various factors, including jaw injury, teeth grinding (bruxism), arthritis, and stress. Treatment for TMJ disorders may include lifestyle modifications, dental appliances, physical therapy, stress management techniques, and in severe cases, surgery to repair or replace the affected joint.
4. Trigeminal Neuralgia:
Trigeminal neuralgia is a chronic pain condition that affects the trigeminal nerve. Which is responsible for transmitting sensations from the face to the brain. Individuals with trigeminal neuralgia experience sudden, intense facial pain that can be triggered by activities such as eating, talking, or touching the face. The pain is often described as stabbing, shooting, or electric shock-like in nature and can be debilitating. Treatment for trigeminal neuralgia may include medications, nerve blocks, and surgical interventions to relieve pain and improve quality of life.
5. Facial Trauma:

Causes of facial pain
Facial trauma, such as fractures, bruises, or lacerations, can cause significant pain and discomfort in the affected area. Common causes of facial trauma include falls, motor vehicle accidents, sports injuries, and physical assaults. Depending on the severity of the injury, treatment may involve rest. Pain management, wound care, and in complex cases, surgical repair or reconstruction to restore facial function and appearance.
Summary
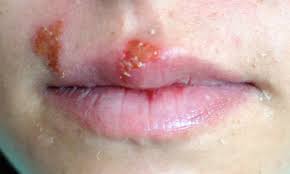
Dental problems (abscesses), infections (herpes zoster, sinusitis), nerve diseases (trigeminal neuralgia), and TMJ (temporomandibular joint) abnormalities are frequently the cause of facial pain. It frequently radiates from the jaw, teeth, or sinuses and can feel like scorching, dull ache, or strong electric shocks. Salivary gland issues, face traumas, and migraines are further causes.

 Social media2 weeks ago
Social media2 weeks ago
 Social media1 week ago
Social media1 week ago
 Social media1 week ago
Social media1 week ago
 Photography1 week ago
Photography1 week ago
 Social media1 week ago
Social media1 week ago
 Social media2 weeks ago
Social media2 weeks ago












Pingback: Why Do You Have Too Much Saliva in Your Mouth? - SimplExplainer