
TREATMENT OF ITCHY SKIN
Treatment of itchy skin. In addition to being dry, itchy, or painful, skin rashes can also be red, swollen, and bumpy. Dermatitis, which occurs when your skin reacts to allergens or irritants, is the primary cause. Skin rashes can be caused by bacteria, viruses, allergies, and diseases like psoriasis, eczema, and hives. Numerous therapies can eliminate the rash and alleviate your problems.
TREATMENT OF ITCHY SKIN
The goal of treating itchy skin is to eliminate the source of the itch. Your doctor can suggest prescription medication or other therapies if home cures are unable to relieve your symptoms. Managing the symptoms of itchy skin can be difficult and call for ongoing treatment. When skin turns red, swollen, and rough, it’s called a skin rash. Certain skin rashes are painful and dry. Some hurt. A skin rash can be caused by a variety of factors, such as germs, viruses, allergies, and skin disorders like eczema.
Types
Skin rashes come in a variety of forms, including:
1. Contact dermatitis
This type of dermatitis is brought on by your body reacting negatively to a material. Many people have allergies to nickel, which is frequently present in costume jewelry, preservatives, perfumes, and poison ivy. Chemicals, soaps, detergents, and household cleansers are examples of common irritants.
2. Eczema

Also known as atopic dermatitis, eczema typically first appears in infancy and then improves as a child gets older. Genetically, it to run in families. Eczema is also more common in people with allergies or asthma.
3. Hives
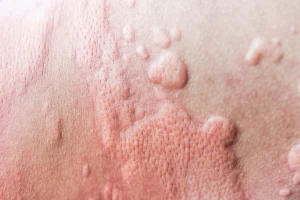
Also known as urticaria, hives are itchy, red, and elevated skin welts. An allergic reaction to insect stings may result in hives. Hives can also be triggered by extreme temperature fluctuations and specific bacterial diseases.
4. Psoriasis

A thick, scaly rash is the result of this chronic skin condition. The rash frequently appears on the scalp, genitalia, lower back, knees, and elbows. It is possible to inherit psoriasis. Viral: A lot of viral diseases, including molluscum contagiosum, measles, and chickenpox, can cause skin rashes.
Signs
The origin and type of skin rash determine the symptoms. One or more parts of the body may get rashes. A rash on the skin could be: Dry. Blistering. Blotchy. Skin discoloration, Blisters, stinging. Scaly or flaky. Like a hive (welts). swelling or inflammatory. Itchy.
Management
The cause of skin rashes determines how to treat them. The rash may not go away for a few weeks. Treatments for skin rashes include: Allergy drugs: One kind of allergy drug that lessens itching is oral antihistamine. Anti-inflammatory lotions: Cortizone and other hydrocortisone creams reduce irritation and inflammation. Immunosuppressants: These medications can lessen the reaction if the skin rash is caused by an immune system reaction or eczema. Its irritation can be reduced by calming it. Oatmeal baths: Dry, itchy skin rashes can be relieved by soaking in a warm bath containing colloidal oatmeal. Check your neighborhood pharmacy for colloidal oatmeal bath products like Aveeno.
Steroids: Your doctor can recommend an oral steroid like prednisone or a topical steroid cream if your symptoms don’t go away. Steroids reduce itching and inflammation. Topical immunomodulators: These drugs alter (modulate) how your body reacts to allergens. Tacrolimus ointment and pimecrolimus skin cream are examples of prescription drugs.
Summary
A skin rash’s impact on your life is mostly determined by its cause. You can avoid allergens and irritants that you know cause you discomfort, but viruses and bacteria are difficult to prevent. Most rashes, regardless of their etiology, are bothersome but manageable. Certain skin disorders, such as psoriasis, require extra attention because they are permanent. The cause of the skin rash might be determined by your healthcare provider. Discuss with your healthcare professional ways to reduce exposure to triggers that cause rash. To address your unique symptoms and rash type, your provider can create a personalized treatment plan.

 Photography4 weeks ago
Photography4 weeks ago
 Social media4 weeks ago
Social media4 weeks ago
 Music4 weeks ago
Music4 weeks ago
 Social media4 weeks ago
Social media4 weeks ago
 Business3 weeks ago
Business3 weeks ago
 Social media3 weeks ago
Social media3 weeks ago































Pingback: Slippery Elm Ointment: Uses and Benefits - SimplExplainer
Pingback: The Effects of Tattoos on the Body and Mind - SimplExplainer