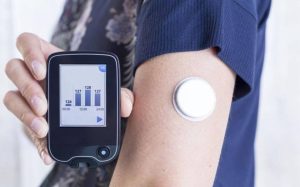
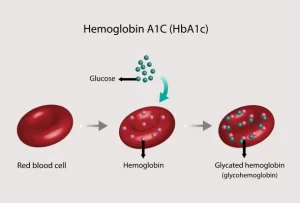
Monitoring diabetes. Red blood cells include a protein called hemoglobin, which is in charge of distributing oxygen throughout the body. Glycated hemoglobin is created when glucose, or sugar, binds to hemoglobin after entering the bloodstream. The average blood glucose content over a three-month periodcthe normal lifespan of a red blood cell—is directly correlated with the amount of glycated hemoglobin that is produced. One essential metric for identifying and managing diabetes is glycated hemoglobin, or HbA1c. The definition, significance, measurement, and consequences for diabetics of glycogen hemoglobin will all be covered in this article.
MONITORING DIABETES
Because it offers a long-term perspective on blood sugar control, HbA1c is an essential tool in the diagnosis and treatment of diabetes. People with diabetes can greatly lower their risk of problems and enhance their general quality of life by being aware of the importance of HbA1c and managing it proactively. A thorough diabetes treatment strategy and routine monitoring are essential for reaching and sustaining ideal HbA1 levels.
Significance of glycated hemoglobin;
1. Diagnosis of Diabetes
• The HbA1c test is used to diagnose prediabetes and diabetes. A higher glycated hemoglobin level indicates poorer blood sugar control and a higher risk of diabetes-related complications.
2. Monitoring Blood Glucose Control
• For individuals already diagnosed with diabetes, the test is a reliable measure of how well blood sugar levels have been controlled over time. It helps in assessing the effectiveness of diabetes management plans, including medication, diet, and exercise.
3. Predicting Complications
• Persistent high levels of glycated hemoglobin are associated with an increased risk of complications such as cardiovascular disease, neuropathy, nephropathy, and retinopathy. Therefore, maintaining an HbA1c level within the target range is crucial for reducing these risks.
How is HbA1c Measured?
The HbA1c test is a simple blood test. It doesn’t require fasting and can be done anytime of the day. The test is usually run in a lab, but point-of-care testing kits can also be used in clinics and, in certain situations, at home.
Understanding glycated hemoglobin Results;
– Normal Range
– An HbA1c level below 5.7% is considered normal.
Prediabetes
• An HbA1c level between 5.7% and 6.4% indicates prediabetes, suggesting an increased risk of developing diabetes.
Target HbA1c Levels;
For individuals with diabetes, the target level may vary depending on several factors, including age, duration of diabetes, presence of other health conditions, and individual patient factors. Generally, the American Diabetes Association (ADA) recommends a target HbA1c of less than 7% for most adults with diabetes.
Factors Affecting HbA1c Levels
1. Blood Sugar Control
• Effective management of blood glucose levels through medication, diet, and exercise is crucial for maintaining a desirable level.
2. Red Blood Cell Lifespan
• Conditions that affect the lifespan of red blood cells, such as hemolytic anemia or recent blood transfusions, can impact it’s results.
3. Other Medical Conditions
• Conditions like chronic kidney disease or liver disease can also affect it’s levels.
Tips for Managing HbA1c Levels;
1. Regular Monitoring
• Regularly check blood glucose levels and have HbA1c tested as recommended by your healthcare provider (usually every 3-6 months).
2. Healthy Diet
• Follow a balanced diet rich in whole grains, fruits, vegetables, lean proteins, and healthy fats. Limit intake of sugary foods and beverages.
3. Physical Activity
• Engage in regular physical activity, such as brisk walking, swimming, or cycling, to help control blood sugar levels.
Summary
By using a blood glucose meter or continuous glucose monitor to examine blood glucose levels, diabetes can be monitored and the effects of food, exercise, and medication can be better understood.

 Social media2 weeks ago
Social media2 weeks ago
 Social media1 week ago
Social media1 week ago
 Social media1 week ago
Social media1 week ago
 Photography1 week ago
Photography1 week ago
 Social media2 weeks ago
Social media2 weeks ago
 Social media1 week ago
Social media1 week ago