IUD side effects. Even though IUDs are a practical and efficient method of birth control, people can make better choices if they are aware of any possible negative consequences. To make sure the IUD is operating properly and to address any side effects, routine follow-ups with a healthcare practitioner are crucial. It is important to get medical help right once if any serious or worrisome symptoms appear.
IUD SIDE EFFECTS
A medical professional inserts an IUD (Intrauterine Device), a tiny, T-shaped, long-acting method of reversible birth control, into the uterus. Depending on the type, it can last for three to twelve years and is more than 99% efficient at preventing conception. Like any medical equipment or medication, intrauterine devices (IUDs) might have negative effects, but they are a very effective long-term form of contraception. These are five typical IUD side effects:
1. Irregular Bleeding and Spotting;

Description: Many women experience changes in their menstrual bleeding patterns after IUD insertion. Hormonal Intrauterine Devices (such as Mirena, Kyleena, and Liletta) can cause irregular bleeding and spotting, particularly in the first few months. Over time, periods may become lighter and less frequent, with some women experiencing amenorrhea (complete absence of periods). Copper IUDs (such as ParaGard) often cause heavier and longer periods with more intense menstrual cramps, especially initially
Management: These symptoms usually improve after the firt 3-6 months. If bleeding is severe or persistent, it’s important to consult a healthcare provider.
2. Cramping and Discomfort;
Description: Insertion of an IUD can cause cramping and discomfort, which may last for a few days to a few weeks. Some women may also experience cramping during their periods or at random times while the IUD is in place.
Management: Over-the-counter pain relievers such as ibuprofen can help manage cramping. If pain is severe or persists, it is advisable to seek medical advice.
3. Risk of Infection;
Description: There is a small risk of infection associated with the insertion process. This risk is highest within the first 20 days after insertion. The infection can occur if bacteria are introduced into the uterus during the procedure.
Management: Following proper aseptic techniques during insertion minimizes this risk. Symptoms of infection, such as fever, severe pain, or unusual discharge, should be promptly evaluated by a healthcare provider.
4. Expulsion;
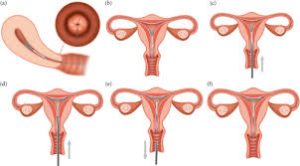
iud side effects
Description: The IUD can be partially or completely expelled from the uterus. This is more likely to occur in younger women, women who have never been pregnant, or shortly after childbirth or abortion. Expulsion can reduce the effectiveness of the IUD and may require re-insertion or a different contraceptive method.
Management: Regular self-checking of the IUD strings (as instructed by a healthcare provider) can help detect expulsion. If the IUD is expelled, it is important to use backup contraception and contact a healthcare provider.
5. Hormonal Side Effects;
iud side effects
Description: Hormonal IUDs release levonorgestrel, which can cause side effects similar to those of other hormonal contraceptives. These may include:
– Acne
– Breast tenderness
– Mood changes, such as depression or irritability
– Headaches
– Nausea
Management: These side effects often improve over time as the body adjusts to the IUD. If side effects are bothersome or persistent, discussing alternatives with a healthcare provider is recommended.
Summary
The type of IUD has a significant impact on its negative effects. Headaches, mood swings, and irregular bleeding are common side effects of hormonal IUDs (such Mirena and Kyleena). Although hormone-free, copper IUDs (like Paragard) frequently exacerbate monthly cramps and bleeding.