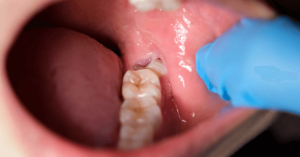
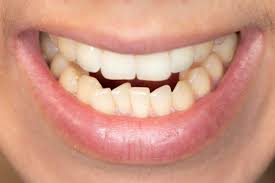
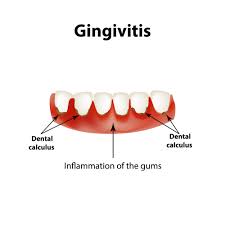
Analysing gingivitis. This is a common and moderate form of gum disease (periodontal disease) that causes irritation, redness, and swelling (inflammation) of your gingiva, the area of your gum around the base of your teeth. Gingivitis is a prevalent, reversible, and non-destructive form of periodontal disease characterized by inflammation of the gums (gingiva). Bacterial plaque, a sticky layer of germs that develops on teeth,
ANALYSING GINGIVITIS
is the main cause. Gingivitis can develop into periodontitis, an irreversible disease that causes bone and tissue loss and can result in tooth loss, if treatment is not received. The most typical signs include bleeding, especially when brushing or flossing, and red, puffy, or swollen gums. Tenderness and bad breath (halitosis) are other symptoms.
Key symptoms:
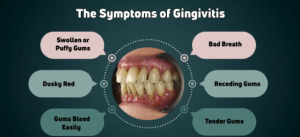
1. Gum Redness: The gums become red and may appear swollen.
2. Bleeding Gums: Gums may bleed, especially during brushing or flossing.
3. Bad Breath: Persistent bad breath, also known as halitosis, can be a symptom of gingivitis.
4. Tender or Sensitive Gums: Gums may be tender or sensitive to the touch.
5. Receding Gums: In some cases, gingivitis can cause gums to recede, making teeth appear longer.
Gingivitis is often caused by the accumulation of plaque — a sticky film of bacteria — on teeth and gums. Poor oral hygiene is a primary factor, but other factors such as smoking, certain medical conditions, and hormonal changes (as seen in pregnancy, menstrual cycle, or menopause) can contribute.
More symptoms;

Gingivitis can often be effectively treated and even reversed with proper oral hygiene and lifestyle changes. Here are key steps for managing and curing gingivitis:
1. Improved Oral Hygiene:
– Brush your teeth thoroughly at least twice a day with a fluoride toothpaste.
– Use a soft-bristled toothbrush to avoid irritating your gums.
– Floss daily to remove plaque and debris between teeth.
– Consider using an antiseptic mouthwash as recommended by your dentist.

2. Professional Dental Cleanings:
– Schedule regular dental check-ups and professional cleanings to remove accumulated plaque and tartar that may be difficult to reach with regular brushing and flossing.
3. Address Underlying Factors:
– Quit smoking if you smoke, as smoking can contribute to gum disease.
– Manage any underlying health conditions that may be affecting your oral health.
4. Balanced Diet:

ANALYSING GINGIVITIS
– Maintain a balanced diet rich in vitamins and minerals to support overall oral health.
5. Avoiding Irritants:
– Limit alcohol consumption.
– Be cautious with certain medications that may cause dry mouth, contributing to gingivitis.
6. Stress Management:

ANALYSING GINGIVITIS
– Manage stress, as stress can impact your immune system and oral health.
It’s important to note that the effectiveness of these measures depends on the severity of the gingivitis. If gingivitis progresses to a more advanced stage, known as periodontitis, professional intervention may be required. In such cases, your dentist may recommend scaling and root planing or other periodontal treatments.
Regular dental check-ups are crucial for early detection and intervention. If you suspect you have gingivitis or are experiencing symptoms, consult with a dentist for a proper diagnosis and personalized treatment plan. Stay tuned for more updates.
Summary
The early, treatable stage of gum disease known as gingivitis is brought on by plaque accumulation and manifests as red, swollen, and bleeding gums. Tartar is removed by professional dental cleanings and better oral hygiene (brushing and flossing). If left untreated, it may develop into periodontitis.

 Social media4 weeks ago
Social media4 weeks ago
 Photography3 weeks ago
Photography3 weeks ago
 Music3 weeks ago
Music3 weeks ago
 Social media3 weeks ago
Social media3 weeks ago
 Social media4 weeks ago
Social media4 weeks ago
 Social media3 weeks ago
Social media3 weeks ago