Analysing mouth infections. When pathogenic microorganisms—bacteria, viruses, or fungi—invade the soft tissues, gums, or teeth, it can result in mouth infections, also known as oral infections. Infections can range from slight irritation to serious systemic sickness when the mouth’s complex microbiome is upset by trauma, poor hygiene, or systemic health problems.
ANALYSING MOUTH INFECTIONS
When dangerous germs like bacteria, viruses, or fungus enter and grow inside the oral cavity, it is referred to as a mouth infection. Typical oral infections consist of:
1. Gingivitis:
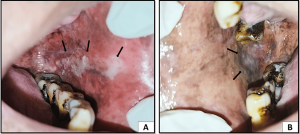
Inflammation of the gums, often caused by plaque buildup. It can lead to redness, swelling, and bleeding gums.
2. Periodontitis: An advanced stage of gum disease involving inflammation and infection that can damage the soft tissue and bone supporting the teeth.
3. Oral Thrush: A fungal infection caused by Candida yeast, resulting in white patches on the tongue, inner cheeks, and throat.
4. Cold Sores:
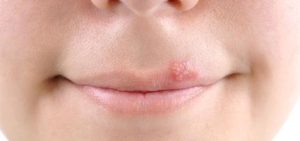
Caused by the herpes simplex virus, cold sores are painful, fluid-filled blisters that typically appear on or around the lips.
5. Canker Sores: Painful, shallow ulcers that can form inside the mouth, often due to factors like stress, injury, or certain foods.
6. Dental Abscess: A pocket of pus that can form within the teeth or gums, usually due to a bacterial infection. It can be extremely painful.
7. Stomatitis:
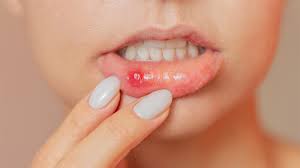
Inflammation of the mucous lining of the mouth, which can be caused by various factors, including infections, allergies, or irritants.
To prevent mouth infections, consider adopting these practices for good oral hygiene:
1. **Regular Brushing:** Brush your teeth at least twice a day with fluoride toothpaste. Use a soft-bristled toothbrush and ensure you reach all surfaces of your teeth.
2. Flossing:
ANALYSING MOUTH INFECTIONS
Floss daily to remove plaque and debris between teeth and along the gumline where a toothbrush might not reach.
3. Regular Dental Check-ups: Schedule regular dental check-ups and cleanings. Your dentist can detect potential issues early and provide professional cleaning.
4. Balanced Diet: Maintain a balanced diet rich in vitamins and minerals. Avoid excessive consumption of sugary and acidic foods, which can contribute to decay and infections.
5. Hydration: Drink plenty of water to help maintain a moist environment in the mouth and to wash away food particles.
6. Limit Tobacco and Alcohol:

ANALYSING MOUTH INFECTIONS
Tobacco and excessive alcohol consumption can contribute to gum disease and other oral health issues. Limit or avoid these substances.
7. Avoid Chewing Tobacco: Chewing tobacco increases the risk of oral cancers and other infections. Quitting can significantly improve oral health.
8. Protective Gears: If you engage in contact sports, wear appropriate protective gear, such as mouthguards, to prevent injuries that could lead to infections.
9. Manage Stress: Stress can affect your immune system and oral health. Practice stress-reducing techniques like meditation or yoga.
10. Avoid Sharing Personal Items:

ANALYSING MOUTH INFECTIONS
Avoid sharing toothbrushes, drinking glasses, or eating utensils, as this can spread infections.
11. Address Dental Issues Promptly: If you notice any signs of dental problems, such as pain, swelling, or changes in your mouth, seek prompt dental care.
By incorporating these habits into your routine, you can maintain good oral health and reduce the risk of developing mouth infections. Regular dental visits play a crucial role in preventive care. Stay tuned for more updates.
Summary
In order to provide individualized treatment programs, dental hygiene analysis is a thorough, data-driven evaluation of a patient’s oral health to detect risks for conditions like gingivitis or cavities. Examining gum health, assessing brushing and flossing methods, and keeping an eye out for tooth grinding are important elements.
Pingback: spit or saliva : It’s role!
Pingback: Why Baby Tooth Matter More Than You Think - SimplExplainer
Pingback: The Benefits of Dental Sealants for Kids and Adults - SimplExplainer